Explant Surgery
 Explant surgery in common terms, refers to removal of breast implant. It has gained increasing prominence due to concerns related to implant safety (implant rupture), implant-related symptoms (Capsular contracture) or diseases resulting form textured-implant (Breast Implant Associated Illness, BII or BIA-ALCL). Goal of this surgery, in most cases, is not only to remove the implant or leaked silicone material but also to remove the capsule (the shell that is made up of scar tissue) around it. Dr. Sabry can help you address your specific issue.
Explant surgery in common terms, refers to removal of breast implant. It has gained increasing prominence due to concerns related to implant safety (implant rupture), implant-related symptoms (Capsular contracture) or diseases resulting form textured-implant (Breast Implant Associated Illness, BII or BIA-ALCL). Goal of this surgery, in most cases, is not only to remove the implant or leaked silicone material but also to remove the capsule (the shell that is made up of scar tissue) around it. Dr. Sabry can help you address your specific issue.
What is Capsular Contracture?
Body’s natural response is to form a protective sheath around any foreign body, including breast implants. This is mostly made up of scar tissue (collagen). On occasion, this scar tissue may become hard and tight around the implant causing pain and discomfort and may result in breast deformity. This is termed as capsular contracture. This may also result from implant breakdown and silicone leakage beyond the shell. Capsular contracture is perhaps the most common reason for explant surgery.
What is Breast Implant illness (BII)?
BII is a non-specific constellation of symptoms that may result after breast implant insertion for either cosmetic breast augmentation or breast reconstruction. It can occur with any types of breast implants i.e. Silicone gel-filled, saline-filled, smooth or textured surface, shaped implants etc.
Symptoms may appear soon after surgery or, even years later and they may include,
- Joint and muscle pain
- Chronic fatigue
- Memory or concentration problem
- Breathing difficulty
- Sleep disturbances
- Skin rashes
- Dry mouth and dry eyes
- Anxiety
- Depression
- Headaches
- Hair loss
- Gastrointestinal symptoms
A lot of the symptoms of BII may also be associated with autoimmune and connective diseases such as lupus, rheumatoid arthritis, and scleroderma.
The disease process is still poorly understood. It is still a diagnosis of exclusion, which means that appropriate medical work up should be done for any and all symptoms and, implant should only be considered as a causative factor when a thorough work up is negative. Currently, there is no medical diagnosis for it. However, it is being increasingly recognized and more research is being pursued both by FDA and ASERF, Aesthetic Surgery Education and Research Foundation.
It is also important to know that in many cases, and NOT all, symptoms may improve or disappear after the implant is removed along with the capsule.
Is Explant Surgery Right for Me?
Patients who no longer want their breast implants are excellent candidates for explant surgery. Explant surgery is the perfect option for patients experiencing pain, discomfort, or health conditions due to their breast implants.
Candidates must be physically healthy with realistic goals. Ideal candidates for explant surgery are non-smokers with no healing-related issues.
Murray Hill Plastic Surgery & Vein Center Explant Surgery

Explant Surgery Consultations
During your Explant Surgery consultation with Dr. M. Zakir Sabry, he will answer questions you may have about the procedure and will discuss any safety concerns related to the surgery.
What is BIA-ALCL?
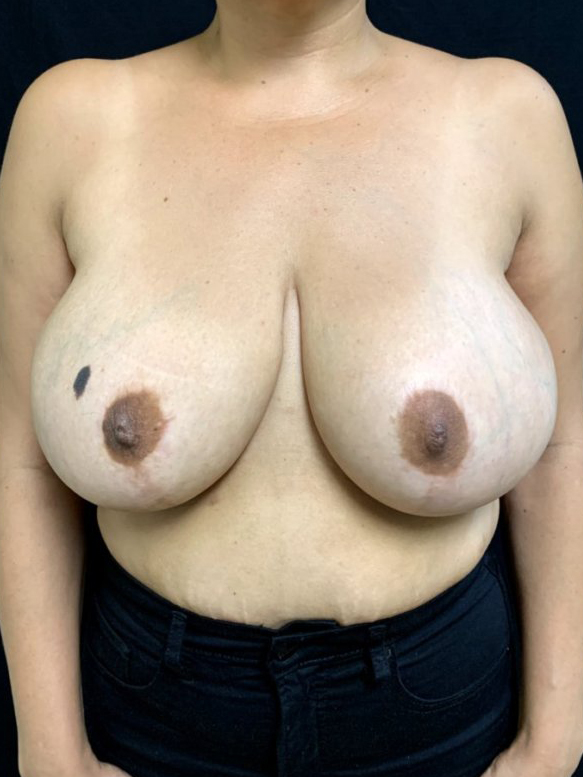
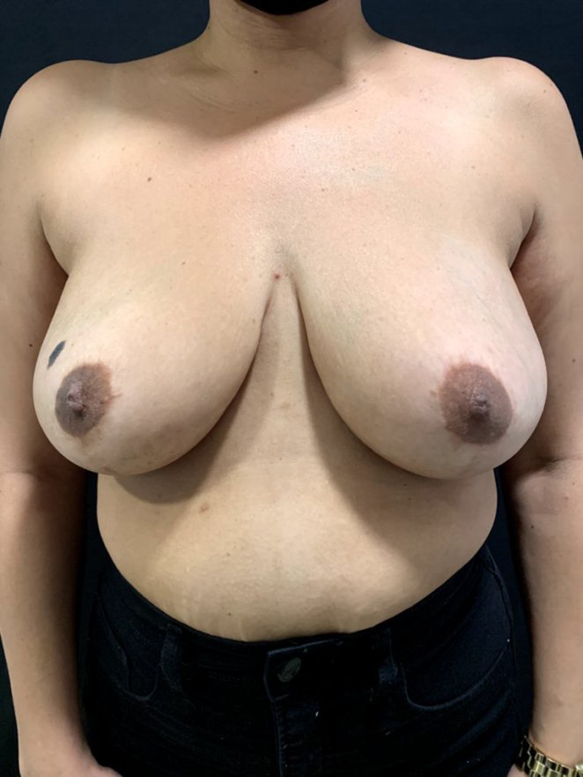
Breast Implant Associated Anaplastic Large Cell Lymphoma is a type of cancer of the immune system that can develop around a breast implant. It is not a type of breast cancer and is a completely different entity than BII. It has ONLY been seen to occur in patients who have had implants with textured surfaces placed either for cosmetic or reconstructive purposes.
Common symptoms of BIA-ALCL include breast asymmetry, breast enlargement, and pain, lump in the breast or armpit, overlying skin rash, hardening of the breast or large fluid collection. Symptoms may appear earliest 1 year after surgery but more commonly in 8-10 years after implantation.
This disease can occur in either patients with silicone or saline implants. Current incidence is 1:2,207 to 1:86,029. Because of varied incidence and lack of significant clinical data, currently, it is not possible to test for who is at risk of this disease.
Work-up
Patients with any of the above symptoms should see their physician at the earliest. Work up should include a PET/CT scan to look for spread elsewhere in the body. An US of the breast followed by a needle biopsy and drainage of the fluid is done next. A special staining (CD30IHC) of the fluid is essential to diagnose BIA-ALCL.
If diagnosed early, the disease is curable with implant removal and capsulectomy (removal of the capsule around the implant).
In advance cases, treatment may include chemotherapy. In rare instances, radiation therapy may be indicated.
How many types of capsulectomies are there and which one should be performed and when?
Capsulectomy refers to removal of capsule ie. Scar tissue that forms around the implant, at the time of explant surgery.
Depending on the type of problem requiring explantation (implant removal), capsulectomies may vary.
- For benign capsular contracture requiring surgery, a partial capsulectomy ie. Removal of the thickest portion of the capsule may suffice. The thin capsule, particularly on the chest wall may be left alone or scored (hatch marked) to promote attaching of the breast flap to the chest wall.
- For Breast Implant illness, a total capsulectomy is warranted. If an implant is found to be ruptured at the time of surgery, then surrounding tissue should be incorporated into the specimen to ensure removal of maximum leaked silicone particles.
- Often, ‘en bloc’ capsulectomy is promoted for most breast implant related surgeries. The en bloc term is often misused when it may truly be a total capsulectomy. The term en bloc refers to removing the capsule and a healthy margin of native tissue around it. This is only indicated for cancer surgeries. Often in social media, the term is used to denote removal of total capsule along with the implant in one piece. The theory is that if an intact capsule is removed along with the implant, one may avoid spillage of silicone material into the native breast or chest wall tissue and remove an intact biofilm. For most surgeons, the en bloc term used in such a way may well just be a great marketing tool. An entire capsule (total capsulectomy) can be removed with or separate form the implant without causing theoretical spillage of silicone material which is deeply embedded in the capsule. For BIA-ALCL, an en bloc capsulectomy must be performed to ensure removal of any and all silicone particles. This can still be done in one piece or separate from the implant.
What to expect during you consultation for breast implant removal?
Dr. Sabry believes in tailoring every surgery based on individual patient’s medical needs and desires. He will explore all your problems, listen intently of your complaints and concerns and thoroughly review your medical history.
After a thorough physical exam and review of records including radiologic findings, he will recommend surgery that best suits your needs. You will be very well informed to make a sound decision and feel confident of your choice.
He will discuss all risks in detail and leave no question un-answered.
The consultation will also include a discussion regarding potential cost of the explant surgery.
The explant surgery procedure
The duration of the explant surgery will depend on the surgical plan and procedures involved.
The breast implant removal procedure will start by administering anesthesia. Once the anesthesia has taken full effect, incisions will be made. Typically, incisions match those of the primary breast augmentation so that no new marks are created.
Next, the breast implants will be removed. In some cases, the scar-tissue capsule will also be removed or altered. The surgery may also include replacing the breast implants according to the surgical plan. Once the necessary modifications are completed, the incisions will be closed using sutures.
The recovery period
The patient’s condition will be monitored before release. Prescriptions will be given for medications, along with specific instructions for a safe and smooth recovery.
The patient will experience temporary bruising and swelling, which will fade during the recovery period. Patients must wear a supportive surgical bra without underwire.
Intense physical activities will not be allowed during the early stage of recovery, including heavy lifting.
What results should I expect after explant surgery?
The final result of breast implant removal surgery will depend largely on the size of the implants being removed and the quantity and quality of your breast tissue remaining. The scar tissue that surrounded your implant ie. Capsule will also play a large role in overall outcome.
Most importantly, if your implant was large compared to the native breast tissue, a breast lift/ mastopexy may be required to address the deflation and droopy appearance. Simultaneous fat grafting can also be performed to add volume. Dr. Sabry will discuss all options at length with you during your consultation. For any revision surgeries, it is imperative that your expectations are realistic and Dr. Sabry will explore all aspects of surgery, postop care, recovery and expectation with you.
Your Explant Surgery will be performed by M. Zakir Sabry MD's surgery center located in New York, NY.







